Is Mesothelioma Difficult to Diagnose?
According to a 2019 Expert Review of Respiratory Medicine article, the early symptoms of mesothelioma are often nonspecific.
Some of these symptoms include persistent coughing, wheezing and shortness of breath. These may resemble signs of the flu or a cold. Doctors may even misdiagnose a patient with a more common illness such as bronchitis.
If you have a history of asbestos exposure and experience these or other symptoms, talk to your doctor right away. Let them know about your asbestos exposure and concerns regarding your risk of mesothelioma.
A mesothelioma specialist also is important because even if your regular doctor considers cancer, they may misdiagnose the wrong cancer. Some patients are misdiagnosed in terms of mesothelioma cell type or given an incorrect cancer stage.
How to Test for Mesothelioma

The diagnostic process for mesothelioma often begins when a patient sees a doctor for a persistent symptom: A cough that never gets better or pain in the chest wall with no obvious cause.
In order to receive a timely and accurate diagnosis of pleural mesothelioma, a patient should seek the expertise of an oncologist, pulmonologist, radiologist, pathologist and surgeon. Cancer centers with dedicated mesothelioma treatment programs have mesothelioma experts in these medical specialties.
Once the patient visits their physician, the doctor may order a chest X-ray or CT scan to investigate further. If the doctor sees something unusual or abnormal in those exams, they may order further tests.
Another route to a mesothelioma diagnosis begins when a tumor is caught by chance on a scan for an unrelated issue. In this case, the patient may have no cancer symptoms.
Either way, most doctors will not suspect mesothelioma unless they know the patient has a history of asbestos exposure. The doctor is even less likely to look for mesothelioma if a person’s asbestos exposure is secondhand.
An example of secondhand exposure is when asbestos workers unknowingly carry asbestos home on their clothing, skin or hair and accidentally expose family members or others in the home.
Can a Chest X-ray Show Mesothelioma?
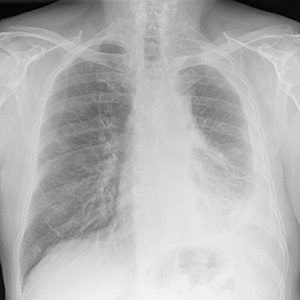
A chest X-ray cannot give a diagnosis of pleural mesothelioma. A radiologist can see abnormal areas on an X-ray, but they will not be able to tell what is causing those abnormalities. They can schedule additional tests to learn more about what is causing symptoms.
CT Scans and MRIs for Mesothelioma Diagnosis
Like X-rays, CT scans and MRIs cannot diagnose mesothelioma. However, they can help the doctor understand the extent and stage of disease.
This information is an important part of planning mesothelioma treatments. It can help identify the best therapies to control the cancer while maximizing quality of life.
Mesothelioma Biopsies
Biopsies can be taken from solid tissue or body fluids. There are several methods for obtaining a biopsy:
- Fine-needle aspiration
-
A surgeon uses a long, thin hollow needle and syringe to obtain cells within or around a tumor.
- Thoracentesis
-
If fluid accumulates in the small space between the lungs and the pleura, thoracentesis can be used to remove the fluid for examination.
- Thoracoscopy
-
A camera-equipped probe inserted through the chest wall helps identify and obtain a tissue sample from any suspicious-looking areas.
- Mediastinoscopy
-
This procedure is like a thoracoscopy, but the probe inserted through the neck instead of the chest.
According to the ASCO 2018 pleural mesothelioma treatment guidelines, cancerous cells should be tested using immunohistochemistry. This identifies the presence and absence of cell markers to confirm the mesothelioma diagnosis and rule out other diseases. No routine genomic tests are currently approved for clinical use. They may be used in research studies or clinical trials.
- Epithelial mesothelioma
- Sarcomatoid mesothelioma
- Biphasic mesothelioma (a mix of both cell types)

Blood Tests for Mesothelioma
Blood tests for mesothelioma look for proteins or other substances present in blood only if a person has mesothelioma. Examples of currently available mesothelioma blood tests include MESOMARK, SOMAmer and Human MPF.
All three tests have advantages and disadvantages. None are yet reliable enough to confirm a pleural mesothelioma diagnosis on their own.
MESOMARK
The MESOMARK test is FDA approved and detects soluble mesothelin-related peptide (SMRP).
SMRP may provide helpful information when monitoring mesothelioma tumor response to treatment, but the test has a higher than acceptable false-positive rate — signaling a person has the disease when they don’t.
There are some cases of false negatives documented as well. A false positive occurs if the test indicates no disease when mesothelioma is present.
SOMAmer
The SOMAmer test evaluates levels of more than 1,300 proteins in blood serum. Using this information, the test is reported to accurately identify mesothelioma in 90 percent of cases. It rules out the disease in 95 percent of people who do not have mesothelioma.
The test appears promising for tracking mesothelioma treatment response, but more data are required to understand if the SOMAmer test will be useful as a stand-alone diagnostic tool.
Human MPF
The Human MPF test looks for megakaryocyte potentiation factor (MPF) in blood. MPF levels increase as mesothelioma tumors grow. This test may be useful for tracking how mesothelioma patients are responding to treatment.
While the test accurately rules out mesothelioma in 95 percent of people who don’t have the cancer, it only catches the disease in 64 percent of people with mesothelioma.
Currently, the test is not sensitive enough to be a useful pleural mesothelioma diagnostic tool.
Additional mesothelioma blood tests are under study. At this time, none of these options are considered accurate enough to replace the gold standard of biopsy-based diagnosis.
How Is Pleural Mesothelioma Staged?
Diagnostic tools help doctors estimate the stage of pleural mesothelioma progression.
There are four stages of pleural mesothelioma. Stage 1 is the least advanced, where surgical removal of tumors is usually an option. Stage 4 is the most advanced, when cancer cells extend beyond the chest to other parts of the body.
Staging is a key part of the diagnostic process because it helps doctors decide whether a patient may benefit from a particular treatment such as surgery or immunotherapy. Staging also helps determine prognosis, survival rates and life expectancy.
Most patients are diagnosed in stage 3 or stage 4 mesothelioma because symptoms typically don’t develop until the cancer begins to spread to nearby organs or beyond the chest wall. Surgery may still be an option at stage 3. Chemotherapy is the most common treatment for late-stage pleural mesothelioma.
How Long Do You Live After Being Diagnosed with Mesothelioma?
The amount of time a person can live after a mesothelioma diagnosis varies from case to case.
Many factors play a role in determining life expectancy for pleural mesothelioma patients, including:
- Stage of disease
-
Stages are 1 to 4 with higher numbers denoting more invasive and widespread disease. Being diagnosed with a more advanced stage typically is associated with shorter life expectancy.
- Other illnesses and conditions
-
A person must be in good general health in order to safely receive certain cancer treatments. Underlying respiratory, kidney or liver problems can make some treatments unsafe for the patient.
- Age
-
In general, younger patients live longer after diagnosis than people who are diagnosed later in life.
- Gender
-
Women tend to fare better than men and have a longer life expectancy after mesothelioma diagnosis.
- Functional status
-
Having the strength to perform usual daily activities, such as taking a walk and completing household chores, is associated with better survival and better cancer treatment tolerance.
Importance of a Second Opinion from a Mesothelioma Specialist
If your doctor is not familiar with asbestos-related diseases, be proactive and ask for a second opinion from a mesothelioma specialist.
It may feel awkward to ask for a second opinion, but it shouldn’t.
This is standard practice in cancer care. Most cancer treatment centers routinely share scans and lab tests with other facilities to help patients obtain a second opinion.
Regardless of where you are in the pleural mesothelioma diagnostic process, seek out a doctor with experience treating the disease. This is one of the most important things you can do to ensure you receive the best cancer therapies for this aggressive cancer.




