What Is Pleural Thickening?
Pleural thickening is a condition triggered by asbestos exposure that causes the pleural lining of the lungs, known as the pleura, to thicken with scar tissue.
This scarring, also known as fibrosis, restricts lung function and may cause chest pain and difficulty breathing.
Treatment involves medication to control pain and inflammation, and pulmonary rehabilitation to help patients breathe easier.
Does Pleural Thickening Mean Cancer?
No, pleural thickening is not a type of cancer, nor is it a sign of cancer. Many people with pleural thickening never develop an asbestos-related disease, but some people do.
Development of asbestos-related pleural thickening means a person was exposed to sufficient asbestos to suffer detrimental health effects. This could mean they experienced enough asbestos exposure to put them at risk of developing an asbestos-related cancer.
Research shows mesothelioma is unlikely to develop in patients with slow-progressing pleural thickening that produces mild pain.
Is Pleural Thickening Serious?
Pleural thickening is a benign condition that is not deadly.
While it is not a cancerous condition, it develops in people who were exposed to enough asbestos to be at risk of developing mesothelioma or lung cancer.
The prognosis with pleural thickening is poor because there is no cure for the condition. Although it is incurable, it is generally not considered life-threatening.

Causes of Pleural Thickening
Prolonged asbestos exposure is a known cause of pleural thickening.
Once inside the body, asbestos fibers migrate to the pleura and cause inflammation, tissue scarring and genetic damage. Pleural thickening is the result of extensive scarring of the visceral pleura, which covers the lungs.
This scarring is believed to be the result of asbestos fibers directly damaging pleural tissue. Researchers have found evidence that asbestos fibers trigger reactive oxygen and nitrogen species, cytokines and growth factor compounds that cause pleural tissue to scar and thicken.
Asbestos Exposure & Pleural Thickening
Approximately 5% to 13.5% of asbestos workers develop pleural thickening. Studies of asbestos workers who developed the condition show most of them worked with asbestos between three and 34 years.
The typical latency period between exposure and diagnosis ranges from 15 to 20 years, but some cases develop within a few years of exposure.
Other Causes of Pleural Thickening
- Coronary artery bypass grafting surgery
- Chronic pneumonia
- Empyema (buildup of pus in pleura)
- Emphysema
- Hemothorax (buildup of blood in pleura)
- Lung infection (such as tuberculosis)
- Pleural effusion
- Pulmonary embolism
- Radiation exposure
- Tumors (malignant and nonmalignant)
These other causes of pleural thickening typically result in the condition appearing on the lining of one lung. Asbestos-related pleural thickening usually affects the lining of both lungs.
Pleural Thickening Symptoms
Scarring, inflammation and restriction of the pleura cause the symptoms associated with pleural thickening.
The condition is marked by extensive scarring of the visceral layer of the pleura. Progression involves scarring that causes the visceral layer to adhere to the parietal layer of the pleura, which lines the chest cavity. This obliterates the space between the pleural layers and may cause significant pain, lung restriction and impairment of lung function.
Diffuse pleural thickening is often preceded by pleural effusion, which is the accumulation of fluid in the pleural space.
Common Symptoms of Pleural Thickening
- Chest pain
- Difficulty breathing and breathlessness
- Tightness in the chest
- Impaired lung expansion and function
- Pleural effusion
Diagnosing Pleural Thickening
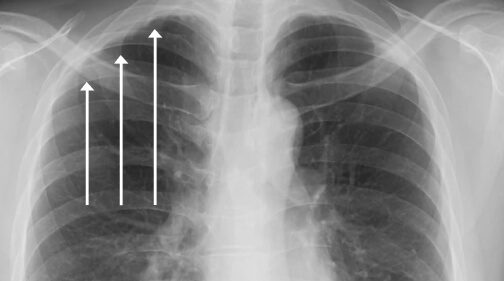
Pleural thickening is diagnosed through imaging scans such as X-rays and CT scans. A biopsy or tissue sample is not required to confirm a diagnosis of pleural thickening.
Imaging Scans to Diagnose Pleural Thickening
- X-ray
- Computed tomography or CT scan
- Positron emission tomography or PET scan
- Magnetic resonance imaging or MRI scan
An X-ray can reveal thickening of the pleura, but a CT scan is more likely to show thickening in better detail. A CT scan, which is also used to diagnose asbestosis and pleural plaques, can confirm the condition earlier.
PET and MRI scans provide even further detail and may be used to differentiate pleural thickening from malignant mesothelioma.
If the cause of pleural thickening is not clear, a biopsy might be taken to see if it shows a cancer such as mesothelioma.

Pleural Thickening Treatment
Pleural thickening cannot be cured, but this nonmalignant condition is rarely fatal, and symptoms are generally not severe. Symptoms are controllable with medication. Pulmonary rehabilitation improves lung function and other treatments provide supportive care.
Treatment for Pleural Thickening
- Medication: Bronchodilators and steroids are prescribed to open airways and reduce inflammation to make breathing easier. Pain medication and nonsteroidal anti-inflammatory drugs are prescribed to alleviate chest pain.
- Pulmonary Function Tests: Tests to measure your lung size and air flow, including spirometry and lung volume tests, will be used to monitor disease progression and direct treatment options.
- Respiratory Aides: Some patients with severe difficulty breathing benefit from oxygen therapy. The type of oxygen therapy recommended to patients will depend upon how much oxygen they need and their accessibility to electrical power. Oxygen tanks are a portable option for patients who need oxygen support and feel well enough to get around.
- Pulmonary Rehabilitation: Pulmonary therapists teach patients how to perform breathing techniques and exercises that help them breathe easier.
- Pleurectomy: While extremely rare, severe cases of pleural thickening have the potential to cause respiratory and cardiac failure. Patients with severe cases may undergo a pleurectomy to remove the lining of the lungs.
- Smoking Cessation: It is extremely important for patients with pleural thickening to quit smoking to improve lung function. Quitting also reduces the risk of developing a separate lung disease.
- Exercise: Research shows people with dust-related diseases, including pleural thickening, benefit from regular exercise. Exercise helps cardiorespiratory function, which strengthens the lungs and improves lung function.
- Complementary Therapies: Other supportive therapies may help patients control pain, such as progressive relaxation techniques, meditation and acupuncture. At-home remedies to reduce pain may include heat or ice therapy and use of the homeopathic topical pain reliever known as arnica.


